
AHIMA is playing a key role in how social determinants of health (SDOH) data is collected, shared, and used. For example, the Data for Better Health initiative provides tools, resources and education to support a better understanding of the importance of SDOH data and how it can be used to improve health and healthcare outcomes. In February, AHIMA released the findings of a study it commissioned on identifying opportunities and challenges with collecting, integrating, and using SDOH data.
Social determinants of health (SDOH) data are valuable in identifying barriers to care and potential interventions. While most healthcare organizations collect this data, research suggests that many struggle to synthesize clinically relevant information into an actionable plan.
Intermountain Health, a not-for-profit integrated health system based in Salt Lake City, UT, has streamlined SDOH data collection, creating alerts in the health record to facilitate real-time interventions and combining the information into accessible dashboards illuminating critical social needs.
The health system is committed to providing affordable, value-based care and achieving health equity by caring for the whole person. AHIMA spoke with Gene Smith, MHA, MBA, community health director for SDOH at Intermountain Health, about how the organization uses social needs data to connect patients with resources and predict social risk.
Q: What types of SDOH data does Intermountain Health collect?
A : It's evolved over time. In 2018, our primary care clinics and hospital emergency departments in Utah began screening Medicaid patients for social needs across several domains, including housing instability, utilities, food insecurity, and transportation as part of a three-year research demonstration project called the Alliance for the Determinants of Health.
: It's evolved over time. In 2018, our primary care clinics and hospital emergency departments in Utah began screening Medicaid patients for social needs across several domains, including housing instability, utilities, food insecurity, and transportation as part of a three-year research demonstration project called the Alliance for the Determinants of Health.
We subsequently expanded social needs screening to include all patients regardless of payer status in our Utah primary care and ED (emergency department) settings. In addition, we developed a separate trauma-informed screening workflow for intimate partner violence that primary care clinics voluntarily adopt. It ensures patients are in a private and safe place when asked these questions, and caregivers receive training on how to assist patients who have or are experiencing partner violence.
Because the Centers for Medicare and Medicaid Services requires hospitals to screen inpatients for all five primary SDOH domains, including interpersonal safety, starting January 1, we're currently working toward implementing screening workflows in inpatient settings.
Q: What has your data shown so far?
A: At the conclusion of the Alliance demonstration project, we learned we could help patients maintain access to primary care services and potentially reduce hospitalizations and unnecessary ED visits by screening for social needs and connecting them to care managers and community health workers. This was significant because the demonstration occurred during the pandemic, when volumes for healthcare services dropped dramatically across the board.
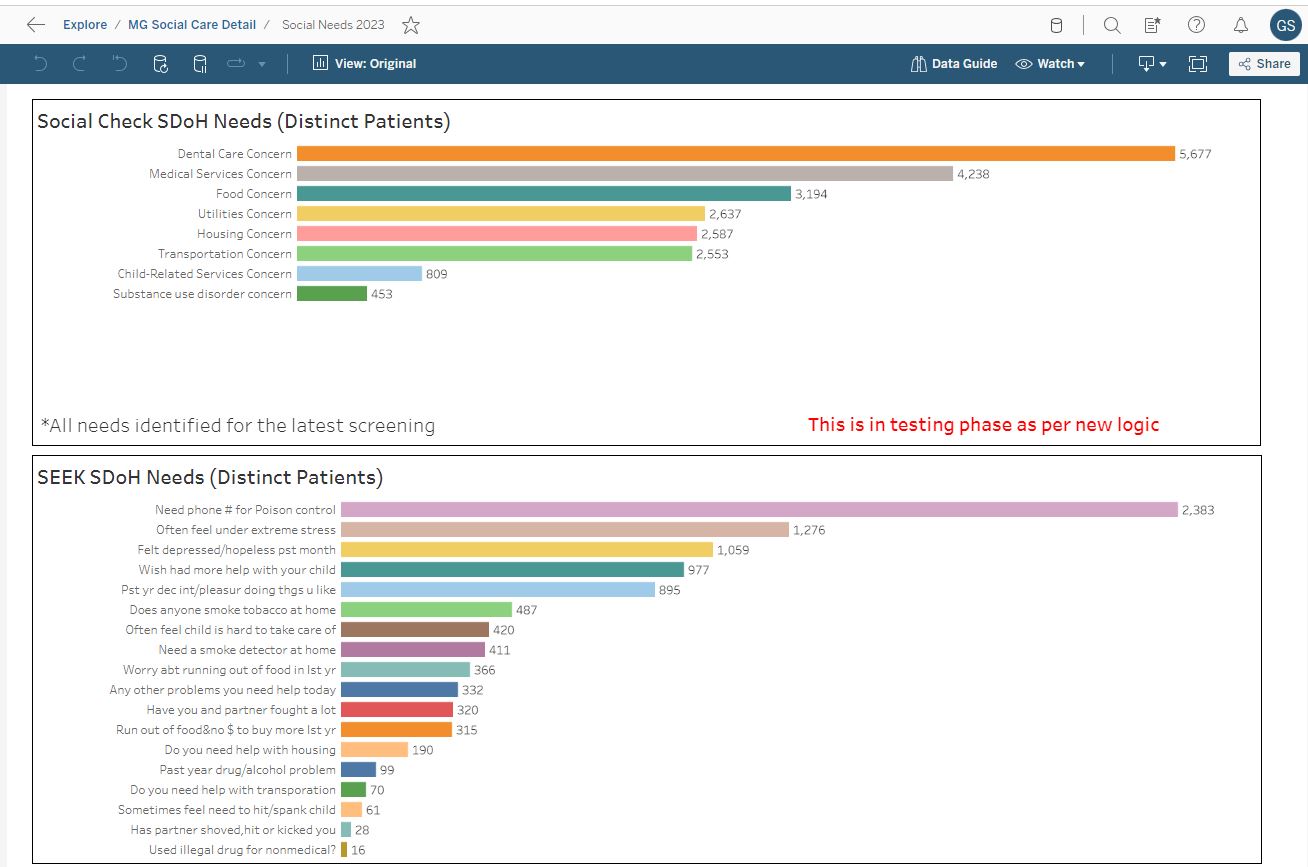
In the bigger picture, we have screened 232,000 patients at the point of care between January and June of this year in Utah, with an average screen-positive rate of 10 percent. Z codes automatically populate in the electronic health record (EHR) for these patients, triggering alerts and reminders for the clinical staff or social needs care coordinators, who then refer patients to community resources and assistance.
We also use SDOH data to predict our health plan members' social risk, so we don't have to wait for them to come into our clinics to identify a need. For this, we focus on food insecurity due to its high correlation with medical risk and outcomes, and call members that the data indicate may be going hungry, validate the need, and connect them to food resources and assistance. We've achieved a 45 percent engagement rate with members, even with cold calling, and found that the predictive data is highly accurate.
Q: What kind of information do the dashboards contain?
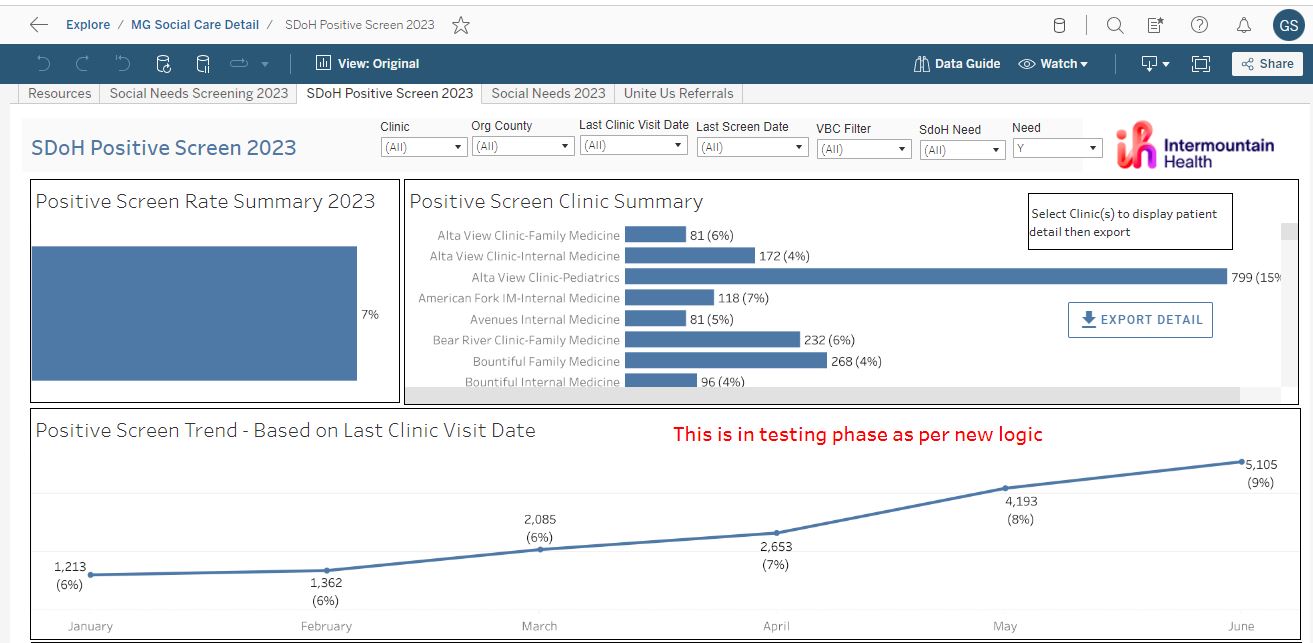
A: Within Utah, we have numerous health equity and SDOH dashboards, including ones that show the percentage of patients screening positive and the affected domains. We also have ones that track the resource referral rates, and our electronic social care referral partner has dashboards showing the accepted resources and resolutions.
Q: What are the greatest obstacles in putting SDOH data into action?
A: Aggregating data from multiple systems. Hospitals and clinics that are connected by one EHR have a more straightforward path to collect data across locations and review it by service, market, or region. But combining data from institutions using several EHRs or systems is hard because they use different screening tools and formats. Overcoming that is key to creating market-specific plans that address an area's prevalent social needs, determining if patients are getting the assistance they need, and identifying where to build more community support infrastructure.
Another obstacle is developing dashboards to show social needs and risk stratifying them, for example, by race, ethnicity, language, and neighborhood, so employees can start developing action plans to systematically address them.
Lastly, allocating staff to collect SDOH information. Initially, having staff conduct screening allowed us to collect data from 35 percent of primary care patients and 14 percent of ED patients. But we received anecdotal feedback that patients are more comfortable divulging certain social needs on a device, like their phone, instead of to another human.
By automating screening, in which health information (HI) professionals play a distinct role, patients now either receive a pre-appointment text with a link to the screening tool or complete a digital ED registration process that includes it. This has more than doubled our participation rates for primary care and pushed the ED screening rate to 70 percent.
Q: How can HI professionals help their organizations collect and utilize SDOH data?
A: HI professionals can assist in creating a standardized, easy-to-administer screening tool and determining a way to automate it through patient-facing digital technologies that don't rely on caregivers to complete. Alternately, they can integrate prompts in the EHR to indicate when a patient needs to be screened and what for, plus add prompts and alerts in the clinical workflow for the care team. It's difficult to contact patients after they leave, so having these reminders populate in real time is important.
HI professionals are instrumental in tracking the free services we extend to patients experiencing social needs, such as food, clothes for a job interview, and computers to take online ESL (English as a Second Language) classes. The government's safe harbors around them are incredibly strict, and HI professionals help us closely monitor those services so we can comply with patient inducement regulations.
Q: Do you have any additional advice for HI professionals?
A: Traditionally, healthcare leadership focuses on clinical needs, but having HI professionals advocate for and prioritize SDOH screening and data aggregation is integral to health equity and giving everyone a fair shot at achieving their best health.
Steph Weber is a Midwest-based freelance journalist specializing in healthcare and law.